What ALARA means — and what it doesn't
ALARA stands for As Low As Reasonably Achievable. It is a core principle of radiation protection, enshrined in the recommendations of the International Commission on Radiological Protection (ICRP) and incorporated into national regulation in virtually every country that practises diagnostic radiology.
The principle states that radiation doses should be kept as low as reasonably achievable, taking into account economic and social factors. That last clause is deliberate. ALARA does not mean using the absolute minimum dose possible for every study — it means using the dose that is appropriate given the clinical purpose, the available technology, the patient's size, and the realistic cost of further dose reduction.
ALARA ≠ lowest possible dose. Reducing dose too aggressively degrades image quality, which can lead to repeated studies, missed diagnoses, or follow-up investigations — all of which increase the patient's total radiation burden. Optimisation means finding the right dose, not the smallest dose.
In practice, ALARA in diagnostic radiology operates through three interconnected activities: justification (is this examination necessary at all?), optimisation (is it being performed at an appropriate dose for the clinical purpose?), and dose limitation (are dose constraints and DRLs being respected?).
This article focuses on optimisation — the middle layer — because it is where day-to-day clinical decisions are made and where dose management data has the most direct impact.
The three pillars of dose optimisation
Protocol design
Setting appropriate scan parameters for each examination type and patient category
Dose monitoring
Continuously tracking actual delivered doses and comparing them to DRL benchmarks
Review & feedback
Structured review cycles that translate dose data into protocol changes
Protocol design: where optimisation starts
Every imaging examination is governed by a protocol — a set of parameters that determines how much radiation is used and how the image is acquired. For CT, this includes tube voltage (kVp), tube current modulation (mA), rotation time, pitch, and reconstruction kernel. For X-ray, it includes kVp, mAs, grid use, and SID.
Well-designed protocols are the foundation of ALARA compliance. A department can have excellent dose monitoring software, but if its CT chest protocol uses 140 kVp and 300 mAs for a routine oncology follow-up, no amount of monitoring will fix the underlying problem.
Protocol design is typically led by the medical physicist working with the radiologist and chief technologist. Key considerations include:
- Patient size stratification — separate protocols for paediatric, standard adult, and larger adult patients. Using an adult protocol on a child is one of the most common sources of unnecessary dose in radiology.
- Clinical purpose calibration — a low-dose chest CT for lung cancer screening has a very different image quality requirement than a CT pulmonary angiogram. They should not use the same protocol.
- Automatic exposure control (AEC) — modern CT systems can modulate tube current based on patient attenuation. Ensuring AEC is enabled and configured correctly is a simple optimisation step that many departments overlook after equipment upgrades.
Dose monitoring: turning data into insight
Protocol design sets the intended dose. Dose monitoring tells you what is actually happening in practice.
The gap between these two can be surprisingly wide. Technologists may accidentally apply the wrong protocol. Equipment may drift over time. A new staff member may override parameters without realising the dose impact. Dose monitoring is the mechanism that detects these deviations before they accumulate into a compliance problem.
Effective dose monitoring requires:
- Automated data collection — manual extraction from modality consoles is too slow and too error-prone to support real ALARA practice. Dose data must flow automatically from the DICOM RDSR into a centralised system.
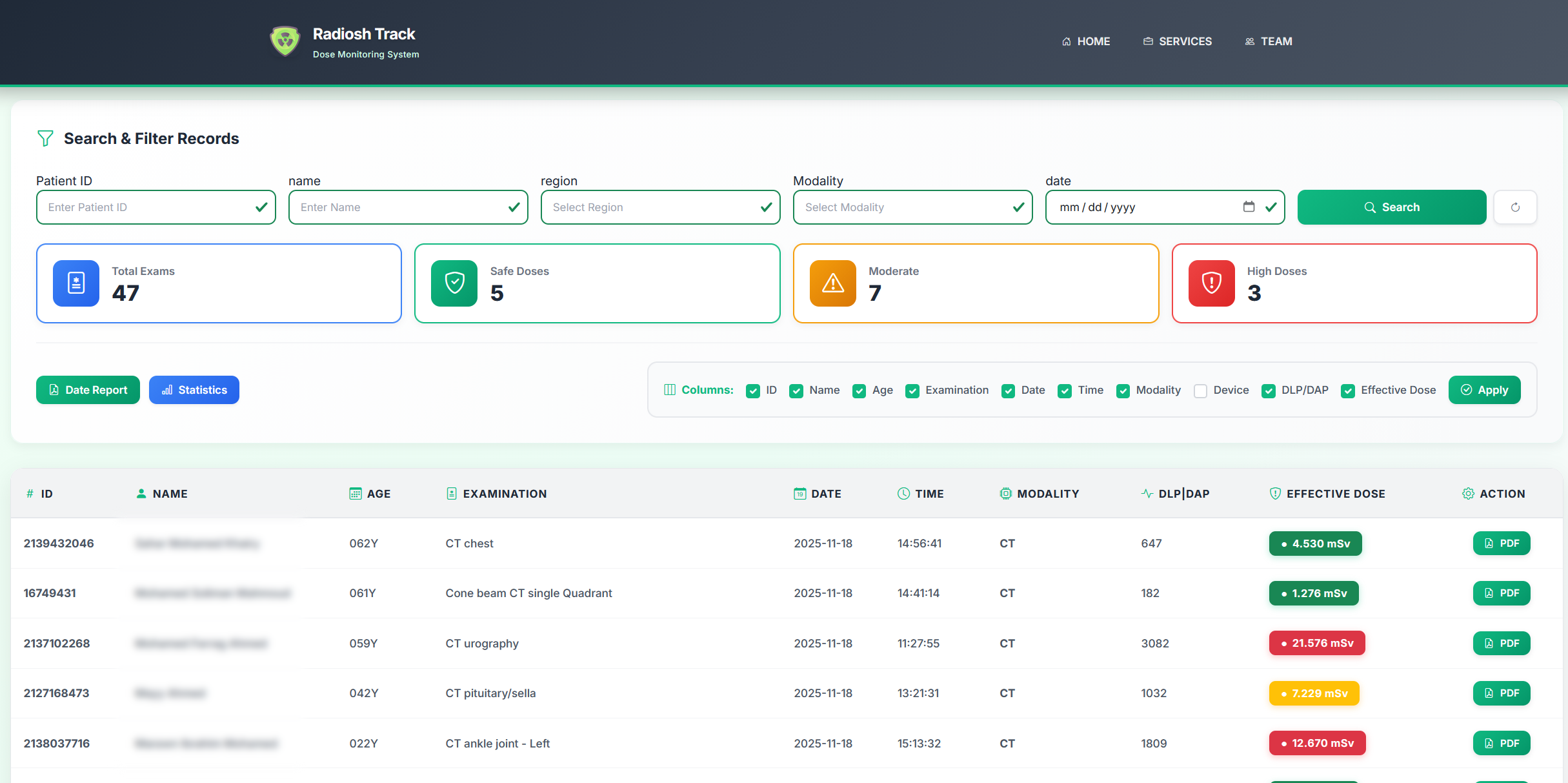
- Patient-level granularity — aggregate statistics can mask individual outliers. A physicist needs to be able to identify specific studies where dose was unexpectedly high, not just know that the monthly average was within DRL.
- DRL comparison — the monitoring system should automatically flag studies that exceed national or local DRLs, and compute running percentile statistics to show where the department sits relative to its peers.
Review and feedback: closing the loop
Data without review is just noise. The defining feature of a department that genuinely practises ALARA — rather than simply citing it — is a structured feedback loop that translates dose data into protocol decisions.
This typically takes the form of a monthly or quarterly dose review meeting attended by the medical physicist, a senior radiologist, and the chief technologist. The agenda should cover:
- Current DRL compliance by modality — are any modalities consistently above the 75th percentile?
- Individual outliers from the past period — were there any studies significantly above DRL? Were they investigated?
- Trend analysis — is dose moving up or down over time? If a protocol was recently optimised, is the dose data reflecting the change?
- Paediatric and special population review — these groups warrant separate attention because they have higher lifetime radiation sensitivity.
The feedback loop is only as good as the data feeding it. A dose management system that generates a two-minute compliance report — rather than requiring a physicist to spend a Friday afternoon in spreadsheets — makes these meetings practical rather than aspirational.
Where ALARA compliance most commonly fails
In our experience working with radiology departments, ALARA compliance tends to break down at one of three points:
1. No baseline dose data
Some departments have never established their own dose distributions. They know their protocols, but they do not know what dose those protocols actually deliver across their patient population. Without a baseline, there is nothing to optimise.
2. Data that is never reviewed
Dose data is collected — perhaps by the PACS vendor's built-in tool — but it sits in a database that no one opens. The data has no feedback channel into clinical practice.
3. Optimisation without documentation
A physicist makes a protocol change following a dose audit. The dose drops. But the change is not documented, the before/after data is not retained, and six months later no one can verify what was done or why. This is a problem both for internal quality management and for external audit.
ALARA is not a one-time exercise. It requires continuous monitoring, periodic review, and documented optimisation cycles. The infrastructure to support those three things is what separates departments that practise ALARA from those that merely reference it.
Key takeaways
- ALARA means the right dose — not the lowest dose. Image quality and diagnostic accuracy are part of the equation.
- The three pillars of optimisation are protocol design, dose monitoring, and structured review.
- Automated dose monitoring is not a luxury — it is the only realistic way to maintain patient-level visibility across a full department workload.
- The feedback loop matters more than the data itself. Data without review cycles does not improve patient care.
- Documentation of optimisation decisions is essential for both internal quality management and external accreditation.